Freeman sheldon syndrome6/2/2023 
The female baby was born in a regional hospital, at term, by emergency cesarean section because of fetal distress and risk of perinatal hypoxia. We obtained the patient's informed consent for publication of the data. The analysis was performed retrospectively basing on the medical records of the patient. We present the course of the disease from the neonatal period to adulthood and discuss the medical problems that were encountered. This report describes a patient with Freeman-Sheldon syndrome. Psychomotor development delay, speech delay Life-threatening respiratory complications and severe respiratory infections Proximal joint involvement (hips, elbows, knees) joint dislocationsĬharacteristic face - prominent supraorbital ridge, sunken eyes, telecanthus, short nose, colobomata of the nostrils weak physiognomical expression “whistling face”įeeding difficulties, dysphagia, failure to thrive, growth deficit Freeman-Sheldon Syndrome - Clinical manifestationsĬongenital contractures of hands and feet (fingers, wrists, ankles) - camptodactyly with ulnar deviation of the hand, talipes equinovarus Table 1 - Clinical manifestations of Freeman-Sheldon syndrome. The most important clinical manifestations typical for Freeman-Sheldon syndrome are listed in Table 1. It is the most severe form of distal arthrogryposis. It should be differentiated from other arthrogryposis syndromes, Schwartz-Jampel syndrome, and trismus-pseudocamptodactyly syndrome (TPS). 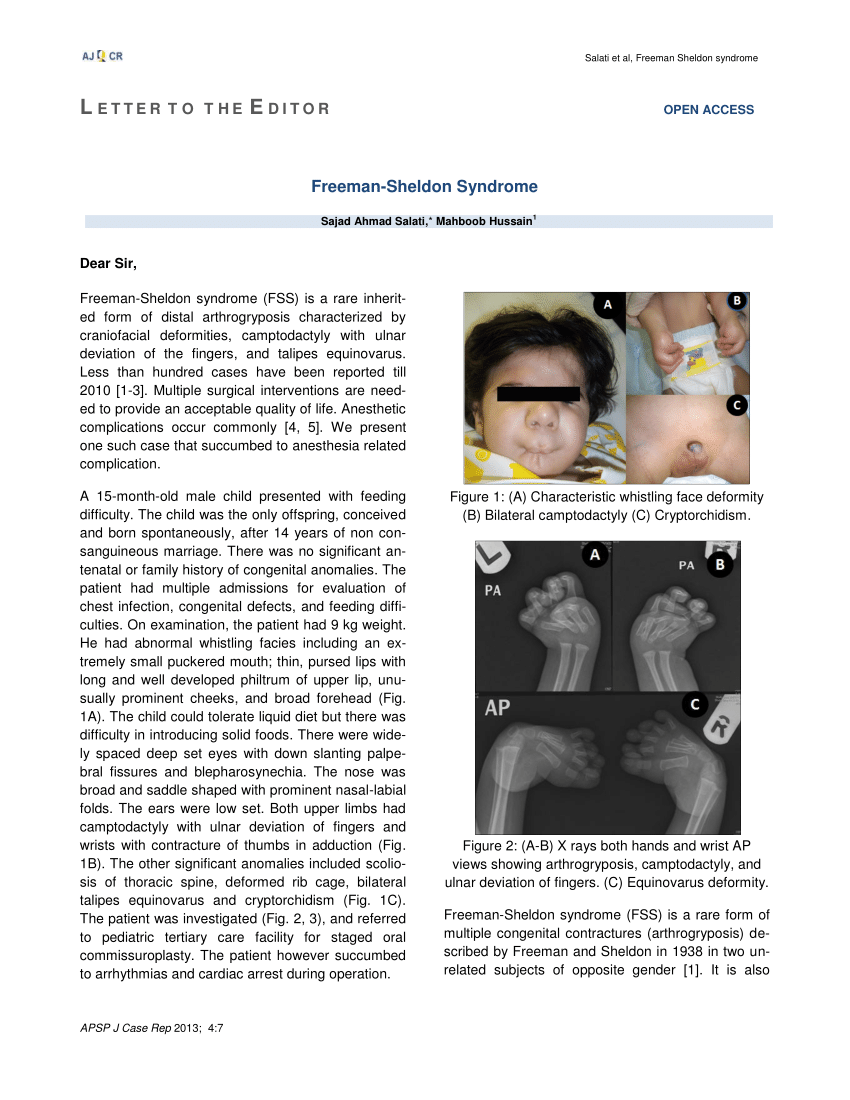
Since the disease shares traits with other MCCs, it is sometimes misdiagnosed, and it is difficult to determine its actual frequency in the general population. It belongs to a group of disorders that are associated with multiple congenital contractures (MCCs), which occur in approximately 1 in 3,000 children. Approximately 100 cases have been reported in the literature so far. įreeman-Sheldon syndrome is a rare disorder that affects males and females in equal numbers. classified Freeman-Sheldon syndrome as a form of distal arthrogryposis with facial abnormality and suggested that it should be called distal arthrogryposis type 2A (DA2A). rediscovered the pathology and called it Whistling Face syndrome due to the fact that microstomia and a scar-like mark extending from the lower lip to the bottom of the chin cause the infants to appear as if they were attempting to whistle. The first two children in whom the disorder was diagnosed had microstomia, facial bone flattening, hypertelorism, small nose and nostrils, finger contractures, ulnar deviation of the hands, and bilateral talipes equinovarus. It is a condition that primarily affects face, hands, and feet. Additionally, the patient had congenital nasolacrimal duct obstruction of the left eye however, a probing and irrigation failed because of obstruction from the abnormal facial anatomy.Freeman-Sheldon syndrome (FSS) was first described in 1938 by doctors Freeman and Sheldon as cranio-carpo-tarsal dysplasia. Eye-opening improved slightly after several weeks of life however, the decision was made to proceed with eyelid surgery to prevent deprivation amblyopia. As is typical for Freeman Sheldon syndrome patients, intubation was difficult and complicated by pneumothorax. When our patient required gastrostomy (G-tube_placement, we performed an exam under anesthesia (EUA)). However, genetic testing confirmed a heterozygous variant in MYH3, consistent with autosomal dominant Freeman Sheldon Syndrome. Although the mode of inheritance for Freeman Sheldon syndrome (formerly known as Whistling Face Syndrome) is often autosomal dominant, our patient had no known family history of congenital abnormalities or consanguinity. The authors describe the findings and management of an infant with Freeman Sheldon syndrome presenting with blepharophimosis of both eyelids resulting in inability to open both eyes during the first several days of life.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
